To learn more about our services and what we can do for you, or to make an appointment, call us today!
Temporomandibular Disorders (TMD or TMJ Problems)
Disease Overview
Temporomandibular Disorders (TMD) is the accepted professional term for TMJ problems, more commonly known to the public as TMJ (Temporomandibular Joint). This constellation of problems is musculoskeletal in origin. It involves either the jaw joints located just in front of the ears and/or the muscles that move the jaw, which are located on the sides of the head. (See Anatomical Illustration on the right.)Although this is a reasonable means of conceptualizing the problem, the disorder is much more complex, involving nervous system and cognitive modifications. This "biopsychosocial complexity" is not unique to TMD. It exists in all medical disorders.
- Pain and dysfunction are the hallmarks of this disease, akin to other musculoskeletal disorders.
- The signs and symptoms can involve just one side (unilateral) or both sides (bilateral) of the head and neck and may include:
- Headaches
- Jaw and/or ear pain
- Teeth pain
- Ear ringing and/or clogged ears
- Neck and/or shoulder pain
- Jaw locking in the open and/or closed positions
- Limited mouth opening (trismus)
- Jaw noises, such as clicking, popping, grinding, or sandpaper sounds
- Teeth clenching or grinding (bruxism)
- Insomnia and dietary restrictions
- Less common symptoms include dizziness, pain in the cheeks and around the eyes, and swallowing pain or difficulty
- Headaches and ear symptoms are frequently misdiagnosed as non-TMD in origin, attributed to sinus problems, ear problems, and migraine headaches.
- Patients commonly attribute their headaches and ear symptoms to sinus problems. They erroneously assume the problem originates in the ears because the jaw joints are located directly in front of the ears, which are affected in most TMD problems. The ear canal forms the back of the TMJs, hence this close anatomical relationship is the reason for this misconception.
- The diagnosis is further complicated by the fact that patients with TMD problems can have most symptoms or a very limited presentation, i.e. just headaches, tooth pain, or ear ringing or stuffiness.
- TMD is a self-limiting problem for most patients. It is generally neither progressive nor degenerative, and patients are uncommonly faced with a lifetime of treatment. If this were not the case, TMD would be endemic in the elderly population. In fact, TMD problems are less common in the elderly and tend to occur at a steady 10% prevalence per decade of life between the age of 20 and 70 years.
- The "gold standard" for TMD diagnosis is a history, clinical examination, and a screening TMJ image.
- Other diagnostic adjuncts, such as electromyography, jaw tracking, sonography, TENS, and sophisticated TMJ imaging, do not improve diagnostic accuracy, and hence, are not recommended.
- Treatment for the average patient includes education, medications, flat plane full coverage occlusal orthotic therapy, and at times, exercises. This treatment regimen is time tested and highly successful, improving or eliminating pain and dysfunction in greater than 95% of patients.
- TMJ surgery is a treatment option indicated for less than 5% of patients. Likewise, orthodontics, bite adjustments, and crowns are not needed for the vast majority of patients.
Problems (Pathologies)
- Most TMD problems are inflammatory and not structural in nature. Inflammatory problems involve either inflammation of the joints, termed capsulitis, and/or of the muscles that move your jaws, especially the muscles that close your mouth, termed myositis.
- Patients with inflammatory problems commonly have bilateral symptoms and do not require invasive therapies, i.e. joint injections, arthrocentesis, TMJ surgery, etc. These problems are generally not structural in nature.
- The most common structural problems include disk displacements and TMJ arthritis. Generally, there are two forms of disk displacement.
- A reducing disk displacement is where the disk is recaptured with mouth opening. Patients with this problem manifest a popping or clicking jaw noise with opening and can generally open fully.
- A non-reducing disk displacement is distinguished by limited opening, deviation of the jaw upon opening to the affected side and pain in the affected joint. Patients with this problem usually had a popping jaw in the past that suddenly stopped popping, accompanied by an inability to open fully (trismus).
- TMJ disk displacements exist in approximately 40% of the general population, are usually well tolerated, and frequently do not result in progression of the disease. Most patients undergo an adaptive intra-articular response after disk displacement, obviating the need to treat the disk displacement.
- Surgical attempts to permanently reposition the disk have high failure rates. Commonly, the disk displaces again and significant side-effects (morbidity) can occur. For a small percentage of patients, the disk displacement is the primary reason for their TMD, associated with frequent closed locking, trismus and/or persisting pain. In such cases, therapies aimed at improving mouth opening and pain are needed. However, even in such cases, TMJ surgery is not commonly needed.
- The third structural problem is arthritic degeneration, usually osteoarthritis accompanied by pain and frequently limited opening. It commonly produces a grinding or sandpaper sound in the joints (crepitus). TMJ arthritis is usually preceded by a non-reducing disk displacement. Because arthritis is commonly a manifestation of host susceptibility, TMD patients with intra-articular arthritis usually have arthritic pain in other bodily joints.
- Other less common TMD pathologies are developmental problems with asymmetrical jaw growth, jaw fractures, and tumors. Benign and malignant tumors are extremely rare causes of TMD.
Causes (Etiologies)
Science has been unable to clearly elucidate a cause for the majority of TMD. Suggested causes include:
- Malocclusions, or bad bites.
- External trauma, i.e. car accidents; blows to the head/neck; etc
Occlusion and external trauma have been shown to be etiologic factors in a very small percentage of TMD patient.
Consistent with the minimal role occlusion plays in TMD, orthodontic care has been shown to neither cause nor cure TMD in large population comparisons. Most malocclusions that correlate with the presence of TMD problems are caused by the TMD problem, as opposed to being the cause of the TMD problems. One's ability to occlude their teeth is determined by jaw joint and masticatory muscle health. For example, TMJ effusions and arthritic changes, along with muscle inflammation or spasms alter the way one's teeth come together. With the exception of boney arthritic changes, these bite changes are transitory and are generally alleviated by successful TMD treatment. The resultant bite changes that occur following significant hard tissue changes in the joints (arthritis) are usually permanent and the most common bite change is the inability to occlude the front teeth.
Bruxism, stress/anxiety, and insomnia. Bruxism is a subconscious clenching or grinding behavior occurring while asleep or clenching during the daytime. Bruxism can be promoted by stress/anxiety and insomnia (co-morbidities).
Of the potential causes, bruxism and stress/anxiety have enjoyed the best scientific support.
- Sleep bruxism is generally of greater consequence than daytime clenching because one can generate greater forces during sleep (up to twice the force generated during eating).
- Sleep partners are generally poor witnesses to the behavior because the period of true observation is usually limited and because clenching is silent, making its more difficult to attest to.
- Diurnal bruxism can be modified by patient awareness, however, nocturnal bruxism is beyond patient control.
- Stress/anxiety is an important risk factor in TMD. Patients commonly recognize that their symptoms occur or worsen during periods of heightened stress.
At times, patients develop TMD problems after a TMD stress that is normally well tolerated, such as routine dental therapies, yawning, eating, etc. It is important to understand that the onset of TMD problems is determined by the relationship of the musculoskeletal insult to stress and bruxism in combination with the patient's ability to accommodate to these insults (host tolerance). Host tolerance is a confluence of factors, such as TMJ remodeling capacity, muscle injury/fatigue tolerance, the ability of the teeth to balance and deflect loading, pain reaction thresholds, etc. When patients are subconsciously loading their muscles and joints, additional musculoskeletal stressors can exceed their tolerance and patients become symptomatic. Hence, the assumed lone initiating factor is simply the final insult, which would not have produced symptoms without the underlying musculoskeletal loading. The role of host tolerance is important to understand in musculoskeletal disorders because this obscure contributor helps explain the quixotic nature of the rheumatologic disease.
Musculoskeletal loading is much greater in one's youth and declines as one ages. However, musculoskeletal pain throughout the body increases with age, even though loading is in decline. The decline in host tolerance factors described previously is the likely reason.
Who Is Affected? (Epidemiology)
TMD affects 5-10% of the population.
- For reasons not clearly understood, women are predominately affected by a 9:1 ratio. The best research to date suggests women are physiologically predisposed, secondary to hormonal influences. The female predisposition also exists in most other rheumatologic/musculoskeletal disorders, i.e. systemic arthritis, lupus, fibromyalgia, etc.
- TMD is uncommon in the very young and very old. Otherwise, the prevalence remains steady for each decade of life. This statistic underscores why TMD is transitory in nature for most patients. It is neither a progressive nor a degenerative condition for most.
Musculoskeletal healing or adaptation is probable for most patients, irrespective of treatment. However, the slow pace of musculoskeletal healing and the persistence of uncontrollable perpetuating factors (stress and bruxism) are reasons why most patients seek care.
Signs and Symptoms
Because TMD is a musculoskeletal problem, signs, and symptoms are defined by pain and dysfunction. As such, patient self-report data plays a large role in diagnosis. Both the presence of disease and the need for treatment is essentially defined by the patient.
Pain
- Qualitatively, it is usually a dull ache, but can be more acute. Also commonly described as feelings of tension, tightness, or fatigue.
- The location is commonly on the sides of the head, either unilaterally (on one side) or bilateral (on both sides).
- The frequency can be episodic or constant with varying intensity throughout the day.
- The pain typically worsens with jaw movement or functions, i.e. eating, talking, yawning, and opening wide.
- The presence of pain is determined by patient self-report (historical), palpation findings during a clinical examination (pain with palpation pressure), and pain elicited with jaw movement during the clinical exam.
- The pain can be inflammation and muscle fatigue secondary to bruxism or be the result of intra-articular degenerative changes.
Types of Pain
- Headaches: They are usually tension-type, but TMD can be an initiator for vascular or migraine headaches. The location is commonly on sides of the head but can occur in any location and be generalized. Headaches that are worse during sleep or upon awakening are usually TMD related. The term "tension-type" is a misnomer, as all headaches are probably vascular in origin.
- Facial Pain: Usually in the jaw joints (located in front of ears) and in the masticatory muscles (sides of face). Pain in cheeks and lower jaw are also common. See the illustration below.
- Ear Pain: This is usually referred pain from the TMJs and is secondary to the close anatomical relationship of the jaw joints and ear canals (The ear canals form the back of the jaw joints). Other common ear symptoms include ringing or tinnitus and a stuffy or clogged sensation. Hearing loss and vertigo are sometimes reported, but are uncommon. Patients commonly mistake these ear symptoms as indications of sinus problems, but for most adults, the symptoms are manifestations of TMD.
- Neck/Shoulder Pain: This commonly represents a separate neck problem, i.e. cervical degenerative disease, but can be related to either the TMJ problem contributing to the neck pain or vice versa.
- Toothaches: When associated with TMD, the tooth pain/soreness is usually generalized, variable, and can change locations in the mouth.
Dysfunction
- Joint Sounds: Clicking or popping sounds usually indicate the presence of a reducing displaced disk, though it can indicate a change in the shape of intra-articular tissues. Crepitus or grinding/grating/sandpaper sounds is highly correlated with the presence of TMJ arthritis. Joint sounds in the absence of pain or dysfunction are insufficient to allow the diagnosis of TMD. However, new onset joint sounds or a sudden change in joint sounds can be meaningful and justify treatment.
- Reducing disk displacements do not usually become non-reducing. When the closed locking occurs, it can be episodic and gradual or sudden and permanent.
- An increased frequency of closed locking episodes usually implies that a permanently closed lock is imminent and unavoidable. With a permanent closed lock, patients notice that they suddenly have limited opening, accompanied by pain in the locked joint with the opening. The lower jaw deviates or swings towards the locked joint with the opening.
- Jaw Locking refers to jaws getting stuck in either the open or closed position.
- Open Locking usually results from a combination of TMJ hypermobility in conjunction with contraction of the jaw-closing muscles. In some people, with maximal opening the end of their lower jaw extends beyond a confining bump of bone called the articular eminence. If muscle contraction occurs when the jaw is in this position, it will get stuck open. To spontaneously unlock and re-close requires patients to relax the jaw muscles with massage and/or moist heat. Open locking can be very disquieting causing patients to engage in behaviors to avoid this problem at all cost. They limit opening by stifling yawns and avoiding foods that require wider mouth opening. Sometimes, reduction by a health care professional may be required. This is generally accomplished manually in a dental chair without the need for injections or sedation. The procedure is simple and well tolerated by patients.
- Closed locking usually results from a TMJ disk displacement that the condyle can no longer recapture. Closed locking is usually preceded by jaw popping, i.e. a reducing disk displacement. The popping can continue for months or years before jaw locking occurs. Closed locking usually begins to occur episodically and the patient is able to unlock and resume popping. However, if the locking frequency increases and/or the locking becomes more difficult to resolve, it is probable that the closed locking will become permanent.
- Trismus or limited jaw opening is usually indicative of an intra-articular problem, as opposed to a muscular disorder and can be caused by non-reducing disk displacements or arthritis. The responsible intra-articular pathology can involve an impairment of tissue mobility that exists secondary to reduced joint pressure, diminished joint lubrication, or the formation of fibrous or scar tissue adhesions. Normal opening for most people is 40-50 mm, with a small number of people opening to 50-70 mm. Opening less than 40 mm is considered limited, however, people can generally function normally (eat a normal diet) with an opening above 35 mm. The pain and/or trismus usually causes restrictions in diet and patients commonly avoid eating difficult foods, such as:
- Hard foods, i.e. meat, uncooked vegetables, and chips
- Chewy foods, i.e. gum, candies, jerky, etc.
- Foods that require wide opening, i.e. apples or burgers.
- Bite Changes. Most alterations in patient's occlusion are perceived, but not clinically detectable. These bite changes are transient because they are secondary to muscle and/or joint inflammation or muscle tension. The perceived bite changes generally resolve with resolution of the TMD problem. Bite changes can be secondary to arthritic changes in the TMJs, generally small amounts of condylar bone loss. These bite changes are permanent and remain after other TMD symptoms have been resolved. In these specific cases, occlusal adjustment, evening the bite by adjusting the surfaces of the teeth, is the most cost-effective treatment. Orthodontic care, such as braces and crowning the teeth, are additional solutions with more limited application.
- Sleep disruption (insomnia) can be an important risk factor to TMD because of the relationship between sleep quality and bruxism. Science has shown that when people lighten their sleep, it is accompanied by an "arousal reaction". This is characterized by increases in motor activity (muscular activity), heart rate, blood pressure, and galvanic skin response. The increase in motor activity may involve bodily movement and teeth grinding. People who sleep poorly, i.e. sleep lightly or awaken frequently during the night, grind their teeth more commonly. Patients mistakenly think that sleep disruption is only relevant to TMD if the disruption is because of facial pain. However, the reason for insomnia is immaterial to the facilitation of bruxism. Hence, it does not matter why one sleeps poorly. The important relationship is that poor sleep behavior, no matter the cause, can cause nocturnal bruxism.
- Besides the relationship with bruxism, insomnia can have a negative impact on one's mood, performance, energy levels, etc., hence, sleeping well can have a significant impact on the quality of patients' lives.
- Frequently, and especially in older patients, it is assumed that insomnia is secondary to the need for urination. However, it is probable that these patients awaken for other reasons, and they urinate because the opportunity is there. Patients erroneously form this causative association between the need to urinate and nocturnal awakening because of the obvious temporal relationship, however, such patients are simply unaware of why they awoke. When these patients are pharmacologically allowed to sleep through the night, bedwetting is not an issue, hence the association between urination and awakening is untrue for most patients.
- A very important "take away" message is that insomnia can be caused by many things, such as stress, noise, a partner's snoring, sleeping with pets, trying to listen for children, etc. One reason for insomnia that is very popular today is sleep apnea, which should be ruled out in the presence of other sleep apnea signs and symptoms (gasping for breath during sleep, snoring, and diurnal fatigue). However, it should be understood that most insomnia is not secondary to sleep apnea, and likewise, it is a mistake to indescriminately ascribe the presence of nocturnal bruxism to sleep apnea.
- Obstructive Sleep Apnea (OSA) is a relatively newly recognized disorder. As such, its diagnosis and relevance are presently poorly understood. This is true for the diagnosis and treatment of most "new" disorders. The relevance of most newly discovered problems are usually overstated in the beginning, and it is only with the findings of longitudinal and comparative research that the disorder's diagnosis or treatment can be put in proper perspective. So today, it is fair to say that the relationship of OSA to TMD is likely being overstated.
Diagnosis
The gold standard for TMD diagnosis today is a thorough history, a clinical examination, and a screening radiograph. Expensive, though superiorly detailed, TMJ imaging, such as MRIs and CTs, are neither needed nor recommended for most patients because the information gained has little impact on treatment.
- Patients should avoid extraneous diagnostic efforts, such as TMJ Doppler, TMJ Sonography, EMG (Electromyography), Kinesiography (Jaw Tracking), etc. The test results do not improve diagnostic accuracy and commonly lead to iatrogenic outcomes and unnecessary invasive therapies, such as braces, crowns, occlusal adjustments, and TMJ surgery.
- Caution is advised if you are being told that your jaw is in the wrong place, as determined by jaw imaging, EMG data, analysis of your bite, eccentricities in jaw movement, and/or disk displacements. These assertions are scientifically invalid and commonly lead to prolonged invasive and expensive care, ultimately resulting in iatrogenic injury (unnecessary bite changes).
- Although advances in technology commonly afford more accurate and detailed information, such advances are only meaningful if their therapeutic impact is significant.
Types of TMD Problems (Disease Classification)
Inflammatory Problems
- This is the most common disorder.
- Inflammation of the muscles that move the lower jaw (myositis) and/or the jaw joints (capsulitis) are the common maladies.
- Limitations in jaw movement and jaw locking are uncommon, although disk displacements can be present. If jaws make popping noises for most patients, the disk displacement is unrelated to the pain and dysfunction.
- Pain is present with palpation, jaw movement, and functions, such as yawning, eating, talking, etc.
Disk Displacements
- TMJ disk displacements are generally caused by the stretching or tearing of disk attachments, hence, the displacement is generally permanent and the disk is incapable of returning to its original position. Diminished joint lubrication, adherence of the disk to the hard tissue, and increased joint pressures have also been implicated in the pathophysiology.
- TMJ disk displacements occur in 30-40% of the normal population. They are commonly well tolerated and are not usually associated with pain or dysfunction. For a small percentage of patients, the disk displacement is at the center of the TMJ problem and is responsible for pain, locking, trismus, etc. To be classified as a TMJ problem, the disk displacement must be the cause of pain or dysfunction, i.e. jaw locking, limited opening, dietary limitations, etc.
- Joints with disk displacements may or may not make a popping noise and the presence of popping/clicking generally means the disk is displaced and recaptures with the opening. In this scenario, jaw movement is generally normal. This problem is termed a reducing disk displacement. A non-reducing disk displacement occurs if the end of the jaw (condyle) cannot recapture a displaced disk. In this scenario, joint noise is absent, jaw opening is restricted, and the jaw deviates with the opening towards the joint with the disk displacement.
- Closed locking refers to situations where a reducing disk displacement intermittently becomes a non-reducing disk displacement. In these situations, a patient’s jaw clicks and opens normally most of the time, but at times the disk does not reduce, and the patient is unable to open fully. If the locking increases in frequency and/or becomes harder to unlock, it is probable that the reducing disk displacement will become a permanent non-reducing disk displacement (a permanently closed lock).
TMJ Arthritis
Arthritis refers to breakdown or degeneration of the disk and bone tissues in the joint. Such changes can include thinning of the disk, wearing down of the condyle, and articular eminence hard tissues.
- Arthritis can be isolated to the TMJ, but can also be a manifestation of a systemic joint disease, such as osteoarthritis, fibromyalgia, lupus, polymyositis, etc. Patients, especially young patients, with multi-joint pains (neck, back, knees, hips, shoulders, etc.) should consider an evaluation by a rheumatologist.
- Osteoarthritis is the most common type of TMJ arthritis. Sandpaper-like sounds, grinding, or grating sounds, called crepitus in the jaw joints, generally means that arthritic changes have occurred.
- The significance is age-related, hence some degenerative changes are expected with aging and are normal. Symptomatic TMJ arthritis generally denotes a host susceptibility to articular degeneration, and as such, arthritis commonly exists in other joints (neck, knee, hips, shoulders, hands, and back).
- TMJ osteoarthritis can be asymptomatic, but symptoms include pain, crepitus, and trismus.
- Osteoarthritic changes are commonly preceded by a non-reducing disk displacement. Bite changes can occur when the bone loss in the TMJs is significant. Generally, the associated bite changes include either the inability to occlude one side (if the bone loss is unilateral) or the inability to occlude your front teeth (if the bone loss is bilateral). Such bite changes are permanent and require permanent changes to the teeth in order to correct. These treatments can include bite adjustments, crowns, braces, or TMJ surgery.
TMJ Tumors
They are uncommon and most are benign.
Treatments
For most TMD patients, successful treatment involves a combination of medications, occlusal orthotic therapy, i.e. splint or night guard, and exercises. Medications commonly entail some combination of anti-inflammatory agents (NSAIDs, such as ibuprofen and naproxen and a short course of steroids, i.e. Medrol Dosepak) and hypnotic agents for insomnia.
- These therapies each address different aspects of the disease and are most effective if used conjointly.
- The anti-inflammatory agents (NSAIDs) diminish joint and muscle inflammation, however, the effects are transient as these medicines "chase the problem" and are not preventative. These agents are fine if taken routinely, however, extended routine use should be avoided. Their primary side-effect is gastritis. Meloxicam and celecoxib are the least likely to produce this side-effect.
- The orthotic and the hypnotic agents attack the cause of most people's problems. As such, both are preventative and therapeutic. Regarding orthotics:
- Constant orthotic wear and orthotics that do not cover all of your teeth should be avoided as unneeded bite changes are likely.
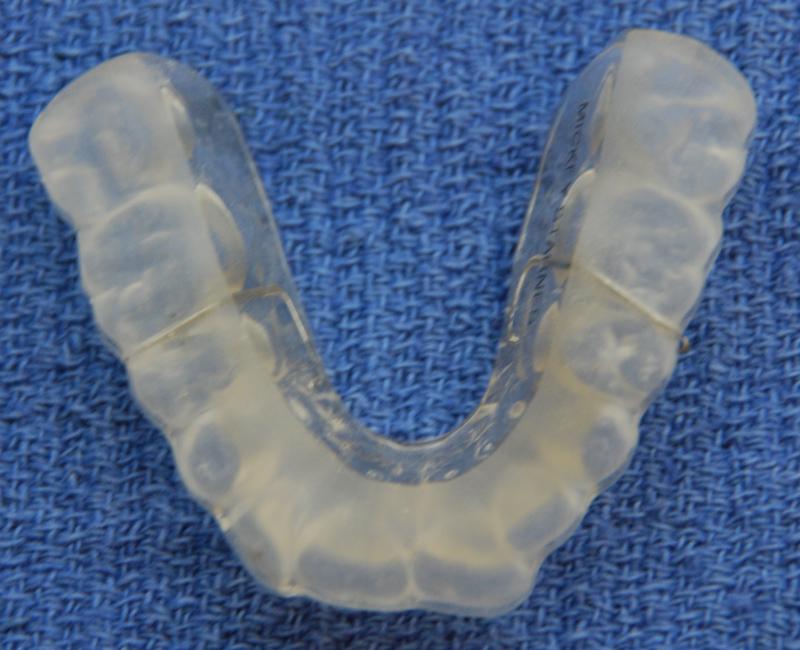
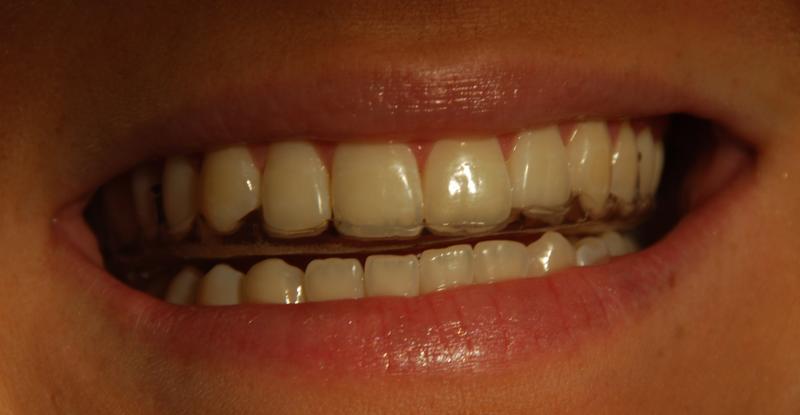
- The problems with over the counter nightguards is that they are made of a soft material which can promote bruxism and do not afford the distribution of loading. The desired orthotic is hard, covers all of your teeth and allows all of the opposing teeth to contact the appliance at the same time.
- Orthotics that fit over the upper and lower teeth are equally effective, however, upper orthotics are preferred because this orthotic best allows the maximum distribution of load (due to the occlusion). The only advantage of lower orthotics is that they are less visible and have less impact on speech, hence are preferred if patients plan to wear the appliance while interacting in public (an unlikely scenario).
- Most patients only need to wear the orthotic at night, but some patients benefit from also wearing the appliance during stressful periods of the day.
- The orthotics that we make are exceptionally durable and can last a lifetime. The appliances can be adjusted and material added to them ad infinitum. (See photographs below.)
- For many patients, their need for the orthotics is long-term, as their bruxism or intra-articular pathology is persistent. However, if one's need for the orthotic is infrequent and predictable, then episodic use is appropriate.
- Regarding hypnotic agents, they can be essential for many patients because poor sleep behavior is a significant risk factor for bruxism. Because the medication is taken at bedtime, addiction is very unlikely. Patients commonly confuse the therapeutic impact of the medication with addiction. For example, the medication will improve your sleep, and if you stop the medication, you will return to sleeping poorly. This is not a manifestation of addiction, but the absence of the medication. It is likened to stopping an anti-hypertensive medication and having your blood pressure increase. Addiction is when one takes a medication for non-medical purposes or unnecessarily escalates the dosing of the medicine. Both of these outcomes are unlikely with taking a medication at bedtime for sleep. With all treatments, patients' compliance depends on their risk-benefit assessment. If the risks are low and the benefits significant, compliance is sensical.
- Generally irreversible and invasive TMD treatments should be avoided, such as occlusal adjustments, braces, crowns, and surgery. Bite adjustments, full mouth rehabilitation, and braces are not recommended for most patients because one's bite (occlusion) and the position of one's teeth are unrelated to most TMD problems.
- TMJ corticosteroid injections and arthrocentesis (rinsing out the joint) can benefit a subset of patients with intra-articular disorders whose pain/dysfunction are not sufficiently improved with medications, orthotics, and exercise. The indication for a joint injection is a persistent pain with normal ranges of joint movement. The steroid injection is well-tolerated and involves a pressure sensation. We precede the injection with a local anesthetic injection to minimize discomfort. A maximum of three injections is recommended separated by one month each. As with any joint, the benefits of TMJ injections are variable, ranging from complete relief to no long-term improvement. Arthrocentesis only differs from a joint injection by the introduction of a second need to allow the joint to be rinsed out (lavage). This affords the removable of intra-articular inflammatory mediators and helps alleviate negative intra-articular pressure. This procedure is indicated for persistent pain in the presence of limited joint movement.
- TMJ surgery is also rarely needed as a TMJ treatment. For example, our practice evaluates two to four new patients a day and refers fewer than five patients a year for surgery. Most people with structural TMJ problems (arthritis and disk displacements) do not need surgery as an adaptive response is likely with time. Because TMJ surgery has significant failure rates and significant morbidity (side effects), it should only be considered for patients who fail a comprehensive effort at conservative therapy, have untenable pain, and suffer from the dysfunction that is intra-articular in origin. The surgeries include arthrocentesis, arthroscopy, open joint, and joint replacement (artificial joint).
Prognosis
- Most TMD problems are self-limiting and spontaneously resolve over time.
- The vast majority of TMD patients respond to nonsurgical therapies.
- Fewer than 5% of TMD patients require surgery.
- TMD problems can recur. Recurrences depend on environmental factors, such as bruxism activity and external trauma, which are difficult to predict. Recurring problems normally respond to re-instituting nonsurgical therapy.
- A very small percentage of patients suffer from a progressive or debilitating disease.
Insurance Coverage
Medical insurance provides the best coverage for most patients. Few dentists can or do bill medical insurance. TMD providers do not need to be in-network providers for the insurer to pay for care. For a more detailed discussion, see our Insurance Coverage page.

Management of Temporomandibular Disorders
National Institutes of Health Technology Assessment Conference Statement
April 29-May 1, 1996
Conclusions
- There are significant problems with present diagnostic classifications of TMD because these classifications appear to be based on signs and symptoms rather than on etiology.
- Consensus has not been developed across the practicing community regarding many issues, including which TMD problems should be treated and when and how they should be treated.
- The preponderance of the data does not support the superiority of any method for initial management of most TMD problems. Moreover, the superiority of such methods to placebo controls or no treatment controls remains undetermined. Because most individuals will experience improvement or relief of symptoms with conservative treatment, the vast majority of TMD patients should receive initial management using non-invasive and reversible therapies.
- The efficacy of most treatment approaches for TMD is unknown because most have not been adequately evaluated in long-term studies and virtually none in randomized-controlled group trials. Although clinical observation can provide direction, these insights must be followed by rigorous scientific evaluation.
- There is no data to support some commonly-held beliefs. For example, the evidence is insufficient to warrant prophylactic modalities of therapy. Additionally, available data are not persuasive that orthodontic treatment prevents, predisposes to, or causes TMD. Therapies that permanently alter the patient's occlusion cannot be recommended on the basis of current data.
- Although non-invasive therapies are clearly preferred for most TMD problems, in the small percentage of patients with persistent and significant pain and dysfunction who show evidence of pathology, or that an internal derangement of the TMJ is the source of their pain and dysfunction, and for whom more conservative treatment has failed, surgical intervention should be considered.
- The most promising approaches to management and treatment of patients with persistent TMD pain and dysfunction may result from evidence-based practice and patient-centered care. Relaxation and cognitive behavioral therapies are effective approaches to managing chronic pain. Physical therapy approaches need to be scientifically evaluated, as do alternative medicine modalities.
- Future advances in diagnosis and treatment of TMD will occur as the result of multidisciplinary collaborations among a number of fields involving basic and applied science and practice.
- Professional education is needed to ensure proper and safe practice in the treatment of TMD, especially with regard to pharmacological, surgical, and behavioral approaches. Moreover, if patients are to know where to seek help, and if insurance companies are to fully acknowledge the need for treatment of TMD, a consensus must be developed regarding the professional expertise needed to diagnose and treat these serious health problems.
